A decade ago, the patient portal was a breakthrough—a window into your own health record. But in behavioral health, access doesn’t automatically equal engagement.
Our national provider survey revealed that although 70% of leaders believe digital tools are essential, nearly half report that fewer than one in 10 consumers use their portal regularly. The tools may exist—but the relationships they’re meant to support are still missing.
It’s time to rethink what true collaboration looks like. Over the past few months, we’ve been engaging both providers and consumers to help shape a new model for consumer engagement that meets people where they are and keeps them connected across the continuum of care. Keep reading for a Q&A with Dr. Jorge Petit, our chief clinical advisor, to see how the next generation of behavioral health technology is taking shape.
(Editor’s note: The concepts discussed here are based on ongoing research with behavioral health providers and consumers nationwide. Preliminary findings are part of a broader effort to reimagine digital engagement across the continuum of care.)
Q: What are the biggest limitations of current patient portals in behavioral health?
A: Portals available today are a great first step toward transparency. They let you see lab results, request refills, schedule appointments, and message your provider, all of which gives people more control. But when we think about behavioral health, this model falls short.
Historically, patient portals have been built for compliance, not collaboration. They are extensions of the EHR, but they don’t help you stay engaged in your care. In behavioral health, where recovery depends on trust and collaboration, that’s a major gap. We need technology that helps people feel supported between visits—not just informed after them.
Q: Why hasn’t the promise of patient portals been realized?
A: Portals often remain underused because of privacy and stigma concerns, low digital literacy, and limited broadband access in many of the communities we serve. They’re also rarely designed with behavioral health in mind and lack personalized tools, recovery supports, or ways to connect families, peers, and care teams.
Instead, most systems are fragmented across service lines, creating more silos instead of integration. The result is that even when people have access, they rarely use it.
Q: What does a better model for consumer engagement look like?
A: We must move from documenting care to designing mental health client engagement. That means building tools that make participation easy, personal, and continuous. Technology should fit into someone’s life, not just into the provider’s workflow. That might mean mobile access, goal tracking, peer connections, or personalized check-ins that make people feel seen and supported.
Q: We’ve been describing this next step as a “consumer engagement hub.” What exactly is that, and how is it different from a traditional patient portal?
A: If patient portals are transactional, the consumer engagement hub is relational. Where portals provide access to information, the hub creates a continuous, connected experience across the entire behavioral health journey: access, engagement, treatment, recovery, and outcomes.
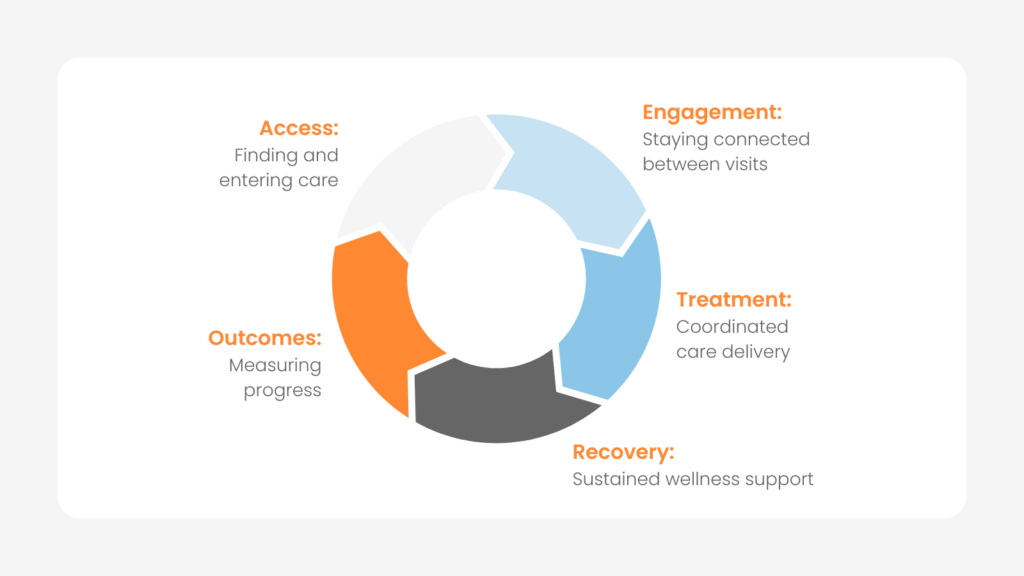
Instead of separate systems for each function, it’s one connected experience designed around people and their support networks. It supports shared decision-making and real-time communication between the individuals being served and their care teams, peers, and families.
Ultimately, a consumer engagement hub transforms care from episodic encounters into a continuous digital relationship.
Q: Where along the behavioral health journey do more comprehensive digital tools like this have the biggest opportunity to make a difference?
A: Our research shows the biggest friction points are at the front door of care—intake, screening, and assessment. That’s where engagement often breaks down. We also see major opportunities in follow-up and monitoring between visits, where people tend to disengage once the initial urgency fades.
The key insight is that the behavioral health journey can’t be episodic. Digital tools can have the biggest impact when they smooth access, maintain connection, and reinforce engagement across the entire continuum of care.
Q: What are the most common barriers to staying engaged between visits and how can technology help close the gap?
A: Simply put, life gets in the way. People are already juggling work, family, stress, and other life demands. They disengage because they lack incentives to stay connected and the system doesn’t adapt to their realities. Technology can help bridge that by offering check-ins, reminders, or supportive nudges that make care fit more naturally into daily routines.
Q: How can digital tools strengthen recovery after treatment ends?
A: Recovery doesn’t stop when treatment does. It’s a process of staying connected. Virtual peer support, telehealth check-ins, and incentive-based tools can help maintain structure and accountability long after formal treatment ends. The goal is to keep people linked to their community of care in ways that feel natural and empowering.
Q: Looking ahead, what are some key themes shaping the future of behavioral health engagement?
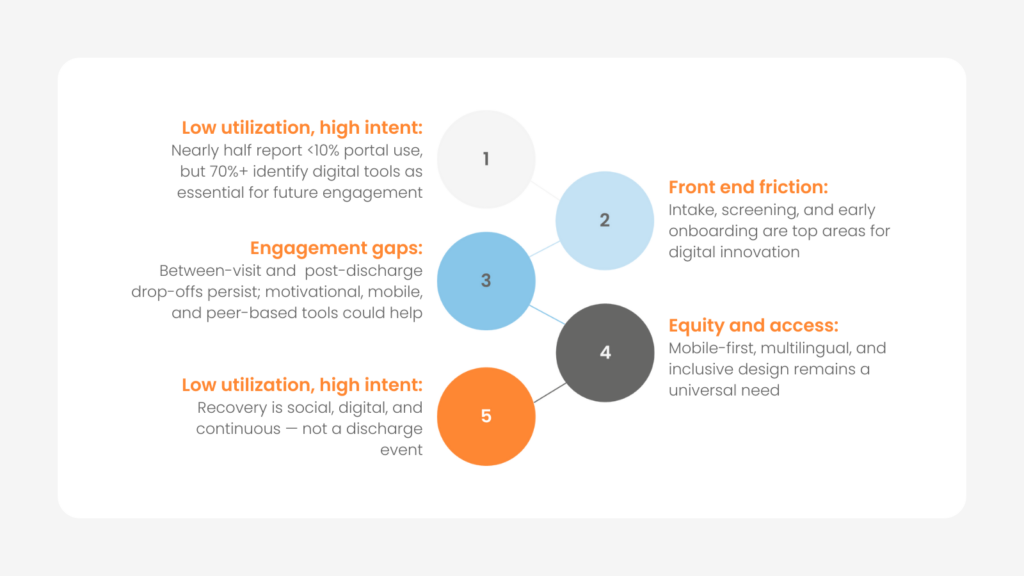
A: Five key themes have emerged that paint a picture of where behavioral health engagement is heading: 1) low utilization but high intent; 2) friction at intake; 3) persistent engagement gaps; 4) the need for equity and access; and 5) redefining recovery. Together, these themes point toward a future that is continuous, personalized, and relationship driven.
Q: How close is Cantata to achieving this vision?
A: We’re well on our way! We ultimately see the consumer engagement hub as an extension of our Arize behavioral health EHR platform that brings together tools like telehealth, digital therapeutics, measurement-based care, and even AI-enabled insights into one connected experience.
We’re building it in partnership with the field—informed by surveys and focus groups that are giving us real insight into where engagement breaks down. While some of this functionality exists today, the full vision is still unfolding as we translate those insights into design and development.
Q: How would you sum up what’s next?
A: If patient portals were the first chapter, what comes next is about partnership and changing the way we show up for people digitally. Behavioral health deserves technology that reflects its humanity, and that’s exactly where we’re headed. We’re learning from providers and consumers to make sure what we build truly meets people where they are.
To dive deeper into Cantata’s vision for the future of consumer access, watch a replay of our webinar Beyond Patient Portals: The Future of Consumer Engagement in Behavioral Health. (Once you register, you will be asked to enter the following passcode: KxwhW1%d)